It’s a dentist! It’s a plane! It’s SUPER-GENERALIST!
I started my practice by leasing space in an existing general dental office. My “landlord” was an accomplished and successful dentist. He told me, “You’ve got to be a ‘SUPER-GENERALIST.'” By that, he meant that a successful general dentist should do most “specialty” treatment himself / herself. Do most of your own endo, perio, oral surgery, complex restorative, etc.
 Over the years, I’ve averaged 50 – 100 hours of continuing education per year. And, over the years, I’ve kept most treatment “in house.” I’ve done most of my own endo, including re-treats. I’ve done my fair share of extractions. And, I’ve done a lot of complex / rehab restorative treatment. I even do short-term cosmetic orthodontic treatment. It has served me well. Patients like “one-stop-shopping.”
Over the years, I’ve averaged 50 – 100 hours of continuing education per year. And, over the years, I’ve kept most treatment “in house.” I’ve done most of my own endo, including re-treats. I’ve done my fair share of extractions. And, I’ve done a lot of complex / rehab restorative treatment. I even do short-term cosmetic orthodontic treatment. It has served me well. Patients like “one-stop-shopping.”
It’s all good, if you feel competent and experienced to handle more difficult cases. However, I submit that the egos of some practitioners may cloud their judgement. Throw in financial pressures, and the GP could find himself regretting the decision to keep certain cases in-house. Ask me how I know! 🙂 Chances are we’ve all been there.
As I’ve aged / evolved, I’m not as “aggressive” as I used to be.
Sometimes ya gotta punt.
The decision to refer to a specialist may not hinge only on the technical challenges presented by the case.  A prudent dentist should also consider factors such as patient management. There are times I’ll refer out a technically “easy” case, simply because I don’t feel comfortable treating the personality attached to the teeth. Getting a social history and getting to know the patient on a personal level can be very valuable!
A prudent dentist should also consider factors such as patient management. There are times I’ll refer out a technically “easy” case, simply because I don’t feel comfortable treating the personality attached to the teeth. Getting a social history and getting to know the patient on a personal level can be very valuable!
Yesterday, I had a new patient that found me through a web search. She mentioned that the reason she chose me over the others was that I had a page with photos and bios for my team. She was in town only for a few months. She and her husband live and travel around the world. And, she was due to leave for Singapore in a couple of weeks.
Her chief complaint was pain on the lower right side. She pointed to both #29 and #30. Her history included sensitivity to cold, hot, and biting.
- Both teeth had been previously restored with crowns (all-ceramic on #29, full gold on #30).
- Clinical inspection revealed good margins on both restorations.
- Percussion was sharply positive on #29 and vaguely positive on #30.
- Cold testing was sharply positive on #30 and a dull, delayed response on #29.
- Palpation in the apical areas was negative.
- Articulating paper revealed an acceptable occlusion, though there are some signs of bruxism.
- The PA radiograph revealed a slight widening of the PDL in #29. The mesial root of #30 was thin and curved, and I couldn’t make out a canal, PDL, or lamina dura. My unscientific description of the mesial root apex is that it appears “fuzzy.”
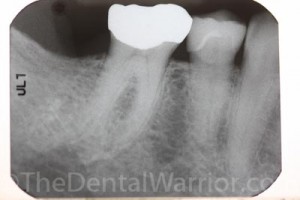 The patient asked me, “Could it be both teeth?” Yep. Could be. But, I’m just not 100% sure of the diagnosis here. I would like to refer you to a specialist with some special equipment (CBCT aka “cone beam”) to dial in the diagnosis.
The patient asked me, “Could it be both teeth?” Yep. Could be. But, I’m just not 100% sure of the diagnosis here. I would like to refer you to a specialist with some special equipment (CBCT aka “cone beam”) to dial in the diagnosis.
Believe me… I could have used the “production.” But, my concern for what’s best for the patient superseded that influence. And, I just knew it would not be an easy case for me. Combine that with the patient’s travel schedule… I just knew I didn’t want to tangle with this particular case.
Endoooooooo!
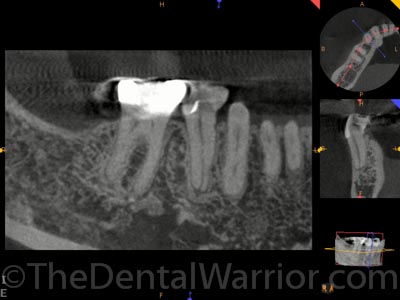 The endodontist was able to get her in right away. They did the CBCT and found that, indeed, both teeth had issues. Both teeth were treated, sealed, and accesses restored by the endodontist. That brings me to another tangential point. Many GPs will get VERY upset if the endodontist restores an endo access with a “core build-up” in anticipation of a crown to be done by the GP (or restores an access in an existing crown). The GP is upset because he or she is missing out on the revenue for the build-up / restoration. I personally believe this is petty and disregards the patient’s interests.
The endodontist was able to get her in right away. They did the CBCT and found that, indeed, both teeth had issues. Both teeth were treated, sealed, and accesses restored by the endodontist. That brings me to another tangential point. Many GPs will get VERY upset if the endodontist restores an endo access with a “core build-up” in anticipation of a crown to be done by the GP (or restores an access in an existing crown). The GP is upset because he or she is missing out on the revenue for the build-up / restoration. I personally believe this is petty and disregards the patient’s interests.
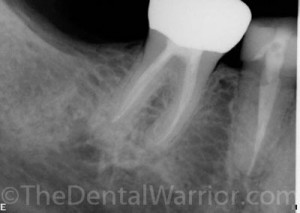 In many cases, the endodontist does place a temporary (Cavit or IRM) and refers back to me for final restorative treatment. However, if the endodontist deems it best to seal the access right then, I have no issue with it. I understand the most common route of re-infection is due to a lack of a coronal seal. Just do what’s RIGHT.
In many cases, the endodontist does place a temporary (Cavit or IRM) and refers back to me for final restorative treatment. However, if the endodontist deems it best to seal the access right then, I have no issue with it. I understand the most common route of re-infection is due to a lack of a coronal seal. Just do what’s RIGHT.
All’s well that ends well.
The patient called us back thanking us profusely for referring her to the endodontist. Sometimes, I have patients that get upset, even begging me to not refer them to “ANOTHER dentist.” But, presented properly in the context of what’s best for the patient, it is always a positive. Also expressing a high level of confidence in the specialist goes a long way.
- “This is the specialist that I sent my own son to for his root canal.”
- “If this was MY tooth, I’d be getting my butt to Dr. Specialist.”
- “Dr. Specialist’s implants look like they grew there.”
Excuse me while I whip this out.
Our specialists can be a fantastic resource, not only technically but in terms of patient management. I have also found that I get a fair bit of referrals FROM specialists. For example, over the years, my periodontists and orthodontists have referred many new patients to me for restorative treatment. Referrals don’t have to be a one-way street.
Don’t be afraid to learn new skills and implement them in your practice. Likewise, don’t be afraid to whip out the referral pad and do what’s best for the patient (and yourself).
 Copyright protected by Digiprove © 2020 The Dental Warrior®
Copyright protected by Digiprove © 2020 The Dental Warrior® 
I referred a patient out to Prosth this week. The patient needed a Pshcologist more than a dentist. There were about 5 RED FLAGS that came up during the toothache limited exam.
PS: Still waiting for the Dental Warrior blog article on getting lower teeth number without the IA block. 🙂
Be thankful for patients that send up the red flags. 🙂
Don’t start stealing my thunder Dr. Mike….
http://www.smartboxwebmarketing.com/pressroom/smartbox-web-marketing-featured-on-cover-of-the-profitable-dentist-winter-edition/
Whatchoo talkin’ about Colin? 🙂
There’s only room for one Superman in dental marketing.
Oh! haha… just looked at the link (cover page photo). I made my “Super-Mike” photoshop many years ago, when someone called me that. I recycle it occasionally. 🙂
I have known quite a few egocentric dentists from my brother’s experience. He has had his fair share with dentists trying to be a hero but ended up being a villain because of greed. They should try to be a dental warrior maybe they can learn a thing or two about doing the right thing. Getting many referrals are signs that you’re a good doctor. My current dentist was actually referred by mom’s doctor. And he gets a lot of referrals from colleagues and patients too. I personally have referred my brother and friends to my dentist because he is a noble dentist worth sharing to the world.
As a patient, it’s great to read words from a dentist who wants what’s best for their patients, not thinking about what they will loose but cares more about the general outcome of the patients dental procedure.