 My friend and fellow dental blogger, Dr. Alan Mead just posted a great article, Don’t just do something, sit there!. In it, he discusses a particular emergency patient he saw recently with whom he couldn’t yet identify a dental issue.
My friend and fellow dental blogger, Dr. Alan Mead just posted a great article, Don’t just do something, sit there!. In it, he discusses a particular emergency patient he saw recently with whom he couldn’t yet identify a dental issue.
Dentists are trained diagnosticians and surgeons. Our prime directive is to find a problem and solve it! Sometimes, when we can’t find the cause of a problem, we STILL want to solve it and do SOMETHING. Alan’s article wisely suggests that sometimes it’s better to do nothing. And, it inspired me to write.
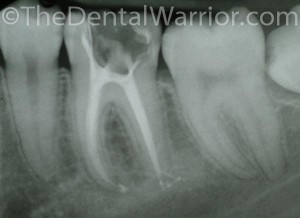 In the day-to-day world of dentistry, most toothaches are successfully eliminated with either root canal treatment or extraction of the offending tooth. And, most times, this is the correct course of action. However, I think some dentists may be predisposed to jumping to that conclusion even in the absence of definitive proof.
In the day-to-day world of dentistry, most toothaches are successfully eliminated with either root canal treatment or extraction of the offending tooth. And, most times, this is the correct course of action. However, I think some dentists may be predisposed to jumping to that conclusion even in the absence of definitive proof.
Sometimes it is a tooth. CTS?
Cracked Tooth Syndrome can be vexing and difficult to diagnose. Duplicating the symptoms is sometimes difficult. Patient descriptions of the symptoms can often be helpful (if you LISTEN). 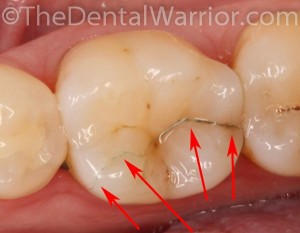 Yet, other times, the patients have a hard time articulating what they’re feeling.
Yet, other times, the patients have a hard time articulating what they’re feeling.
The “Tooth Slooth” is a valuable tool in isolating a tooth that is suffering from CTS and eliciting clinical signs that may lead to a diagnosis. Then you may have to distinguish whether the tooth is cracked or actually split.
Occlusion!
Occlusal issues are often overlooked by dentists, as well. A sensitive tooth may not always be an irreversible pulpitis. I’ve been amazed at how often it’s an occlusal issue. Check occlusion! But, don’t just check centric occlusion. Check excursions, as well. Many disbelieving patients have later thanked me for adjusting the bite rather than doing a root canal or extraction.
Maybe it’s not a tooth.

5 years ago, I got Bell’s Palsy

Fun with Photoshop: Bellvis Palsey!
As my friend, Dr. Alan Mead, mentioned in his blog, a sore upper tooth may be a sinus issue. Accordingly, you may want to consider the rest of the body attached to those teeth, especially when no dental etiology is apparent. The rest of the body can refer pain and other symptoms to the mouth and teeth in a number of ways. If you’re having trouble finding a dental reason for the patient’s complaint, stop and consider that it may not be a dental problem.
To be clear… This blog article is not intended as a complete tome on relating oral signs and symptoms to any and all varieties of systemic medical issues.

 My mission is simply to encourage dentists to think outside the “dental box” when faced with elusive diagnoses.
My mission is simply to encourage dentists to think outside the “dental box” when faced with elusive diagnoses.
A number of medical maladies can refer pain and other symptoms to the oral cavity. Among those are: heart attack, trigeminal neuralgia, Bell’s palsy, burning mouth syndrome, temporal arteritis, Sjögren’s, angioneurotic edema, sinusitis, and even multiple sclerosis.
Keep those in mind when “dental pain” is not accompanied by OBJECTIVE clinical signs or evidence of dental pathology. Don’t treat teeth on a “hunch.” Consider medical issues that may not be dentally related, and consider that the medical issue may be urgent.
An illustrative story….
Several years ago, I had a new patient (a 70-something year old male with a fairly clear past medical history) come into my office in agony. Of all the emergency patients I’ve seen in my career, I’d say this patient’s pain was the most remarkable. He could hardly talk. He pointed to his jaw on the lower left side near the premolar area. He was literally writhing in pain. When I simply touched the area with my hands, he winced. Careful clinical examination with a mouth mirror revealed nothing out of the ordinary. There was no visible decay, inflammation of soft tissues, or swelling. Furthermore, I could not see any damage of any kind to his teeth.
We managed to get some x-rays with great difficulty (due to his pain). The x-rays did not reveal any pathology.
Perplexed by the absence of any obvious dental issues and the degree of his pain, I resorted back to interviewing the patient. I asked the usual “dental” questions about what makes it hurt and what makes the pain go away. No temperature sensitivity. No pain on chewing. It was a constant stabbing pain that could be exacerbated simply by a touch of the hand.
Still getting nowhere with the usual dental questions, I asked a very simple question. It occurred to me that MAYBE this patient had experienced similar symptoms before. And, MAYBE he could tell me what it was.
Me: Have you ever had pain like this… this severe… before?
Patient: Yes.
Me: Tell me about it.
Patient: It wasn’t a tooth problem. It was something else. I can’t remember what it was called. I had to go to a neurologist for an injection (in my head).
Me: Was it trigeminal neuralgia?
Patient: YES! That was what it was called.
Me: How long ago was that injection? (I knew that those alcohol injections last about 5 years)
Patient: About 5 years ago.
Me: You need to see your neurologist again.
It turned out to be a recurrence of trigeminal neuralgia. Unfortunately, these TN patients often go through unnecessary serial root canals and extractions before the proper diagnosis is rendered. Not on my watch! 🙂
Watch and wait
 Sometimes signs and symptoms are vague, and the prudent thing to do is watch and wait. Some aches and pains are idiopathic and fortunately transient. If there is a real, treatable problem, it will eventually become evident. Don’t be afraid to admit you simply aren’t sure what it is and refer to a dental or medical specialist.
Sometimes signs and symptoms are vague, and the prudent thing to do is watch and wait. Some aches and pains are idiopathic and fortunately transient. If there is a real, treatable problem, it will eventually become evident. Don’t be afraid to admit you simply aren’t sure what it is and refer to a dental or medical specialist.
 Copyright protected by Digiprove © 2013 The Dental Warrior®
Copyright protected by Digiprove © 2013 The Dental Warrior® 
Wow! Very nice post! The trigeminal neuralgia case was a huge catch. I’m not sure I would have caught that. You da man!
You started it, Alan! 😉
There’s a good article in Dentistry Today that discusses nonodontogenic etiologies. These can cause a lot of frustration for both the patient and the dentist.
Hi Rob. Thanks for your comments. I think the key is to consider the patient attached to the teeth. Ask questions and listen.
I love this! As an overwhelmed D1, sometimes I wonder why we’re learning all about different diseases and conditions past the mouth. This is why. Glad you actually talked to the patient and were able to identify what the problem was.
Thanks, Yesle. Lots of systemic conditions can manifest signs intraorally. Just remember there’s a whole body connected to those teeth. 🙂
I seriously hope more dentists can think outside their “dental box”…
This is undoubtedly one of the best articles as far as I am concerned. Not very often do you get to read something like this. It is indeed very true that not all dental problems can actually be the problem of the tooth. Dentists must therefore never jump the gun while treating dental problems. Many a times we come across patients writing on blogs that even after root canal their pain has never subsided. Maybe these patient could have been saved from all these pain and suffering if the initial diagnosis was precise. Some dentists have a reputation of that of a money grabber. Maybe its time everyone took a very holistic approach in treating patients.
there are many reasons for a toothache.
pain from surrounding neighbouring structures, mi,senstivity.patient will term senstivity as pain also.
Excellent article! Reminding ourselves to think outside of the box is a must. And it is true not only for dentists or doctors in many field but actually for everyone.
Thank you,
Greg
Emergency Dentist London
“the best dentistry is no dentistry.” … LOVE THIS! It’s true though, it’s very natural to want to figure out what the problem is and it’s absolutely frustrating when you feel “stumped” by what the patient is telling you. I agree 100% though with your conclusion that forcing the issue and performing procedures that may very well be unnecessary could end up doing more harm than good.
It’s nice to read your article, very informative especially on the TN case. Most dentists never could identify such a case.
My dad had jaw pain and went to the dentist. The dentist said nothing was wrong. The next day he died of a heart attack while driving home from work.
Thank you for the article.
This is awful, so sorry for your terrible loss. And well done for spreading the word. I had no idea this could be a sign of heart issues X
As a trigeminal neuralgia patient, I thank you for this article!! So many of us spend years doing unnecessary procedures to try to alleviate the horrific pain. Your article helps!
Thanks! I hope you were able to get some resolution with your TN.
Super post!!!! As a dentist’s wife, an osteopath ( therefore considering occlusion in my diagnosis) but also a patient suffering from trigeminal neuropathy after a dental implant surgery on the jaw ( referred to a dentist friend of my husband) I was complaining from excruciating pain on half of my face, wasn’t listen to….had all my root canaled teeth removed ( on the maxillary area) .before discovering my jaw had been broken during the implant surgery…too late…suffering from iatrogenic Trigeminal neuropathy…no possible surgery, under heavy anti epileptic and other neuroleptic medications, still in excruciating pain and exhausted by too much pain…listen to a patient could have avoid this ( an immediate surgery and pharmacological protocol exist…emergency) . Thank you for your amazing post….indeed the history of the disease is crucial….
Thanks for the nice compliments. Indeed, it’s amazing what information can be discovered with a good history / conversation.
As a TN sufferer, I am so thankful that my dentist knew immediately mine was not a dental issue and referred me to a specialist. I am horrified when I read stories about how other warriors have had teeth pulled and root canals on perfectly healthy teeth. This is such a horrible disease yet very few health professionals know how to diagnose or treat it.
Unfortunately, the adage is sometimes true: “If the only tool you have is a hammer, everything looks like a nail.”
I hope you were able to alleviate your TN symptoms.
After 9 months of annoying pain in my temple,tooth,cheek and behind eye I went to a internist .. took down all the info and said to see my dentist .. did full panoramic view and see nothing wrong under a bridge that has two root canal already.. then go to ER and they do Ct scan on all sinus.. they see minimal mucus give me 10 days of antibiotic.. still have the pain.. was sent to ent they say all look fine.. I’m noticing while I was sleeping my face started hurting and woke me up from the ac… after this I see an eye dr who said eyes are fine.. last resort the neurologist.. had brain MRI .. everything came out fine.. just can’t pinpoint this issue.. but like I said it’s more of an annoying pain that takes your mind off things you have to do each day ..
Other causes of tooth/jaw pain can be food sensitivities (especially nightshades) or B12 deficiencies.
Maybe B12 overdose in my case!? Vegan so 5 weeks ago I decided to mega dose 4,000 a day vs 1,000 B12 bc my blood work showed on the low end of NORMAL! Dumb. Husband was doing also and rash and swelling occurred after slowly over 1 month. I had all over tooth pain and flushing in face like a niacin reaction. Dentist looked, said teeth were fine. Said maybe allergic reaction. General Doctor gave me Claritin to calm allergic reaction. 9 days later still feel allergic reaction AND more extreme teeth pain radiating all over mouth.
Sounds like you have a type of headache called TAC – Trigeminal Autonomic Cephalgia. Of which Cluster Headache is a subtype.
Depending on whether it’s chronic or not, treatment differs. See an orofacial pain specialist for it (preferably a board-certified one)
Indian celebrity bollywood actor was diagnosed with Trigeminal Neuralgia later on when his dentist referred him to neurologist for his underlying tooth pain. Toothache is a common symptom of many oral and systemic diseasdes. Correct Case history is a mandate to pick the early detection of the underlying etiology of toothache.
This was a wonderful article. You reminded us where dentists tend to unintentionally ignore some findings like CTS.
We had a patient who intially came with a badly done incomplete RCT. After repeat RCT also he, kept complaining about pain. We saw nothing in the CBCT. Asked him to go for neurologist consultation, but he was so adamant that the pain needs to be treated by dentist only. After couple of painful months he finally agreed to it and got his “Neuralgia Diagnosed. The awareness among patient is very less and googling has made it impossible for the doctor to tell the patient what is the right course of treatment.
Being a trigeminal neuralgia suffer myself iv had 1top back molar out and 2 bottom ones i am left with 1 lone tooth by itself on my bottom right the pain i have in it is excruciating my dentist cannot see a problem with this tooth but i want it ripped out im due to see my consultant soon as i believe its a tooth problem i went to see an emergency dentist over the xmas period who said the tooth looked ok on xray but was willing to take it out anyway i waited until today to see my regular dentist and he said the tooth was fine!! I also had dry socket on my upper to molar and still feeling pain after 3 weeks could this be referred pain to my bottom tooth?despertley seeking help
Thank you for putting this together, and for doing it just brilliantly.
I thought I was the only one who thought that dentists jump really quick to make conclusions and some of them are too negligent to even look into the root cause of things.
Sometimes the underlying cause is a little different from what you think it may be and that is exactly why a complete check and treatment is important.
For months I have had tooth thropping& pain, dentist took X-rays & says nothing is wrong, the pain is getting more intense, what can I do???
Hi Janet. This blog’s audience is dentists and not intended to be a consumer / patient resource. So, I can’t give any specific advice, since I haven’t seen you as a patient. My general advice would be to find a dentist who can make a diagnosis.
toothache are sometimes uncanny and idiopathic. Just be a patient patient of your dentist in such times.